Voice-to-text tools can cut documentation time by up to 75%, turning 20-minute notes into 3–5 minutes of work. They allow therapists to stay present during sessions, reduce after-hours work, and ensure notes are clear and complete. On the other hand, manual note-taking gives you full control over your documentation but is time-consuming, prone to memory gaps, and often leads to burnout.
Key Takeaways:
- Time Efficiency: Voice-to-text saves 12–15 hours per month, while manual notes take 15–30 minutes per session.
- Accuracy: AI tools achieve 85–95% accuracy, but manual notes allow for capturing subtle non-verbal cues.
- Workflow: Voice-to-text integrates with templates (SOAP/DAP), while manual notes often result in backlogs.
- Client Engagement: Voice-to-text lets you focus entirely on the client, unlike manual methods, which can divide attention.
Quick Comparison
| Factor | Voice-to-Text | Manual Note-Taking |
|---|---|---|
| Time per Note | 3–5 minutes | 15–20 minutes |
| Detail Level | Longer, clearer notes (avg. 320 words) | Shorter notes (avg. 180 words) |
| Burnout Risk | Lower | Higher |
| Client Focus | High | Lower |
| Compliance | Consistent formatting | Variable |
Voice-to-text tools are ideal for busy therapists who want faster, more efficient documentation. Manual notes may still be better for capturing nuanced observations or private psychotherapy records. A hybrid approach – quick session notes manually, formal notes with voice-to-text – might offer the best balance.
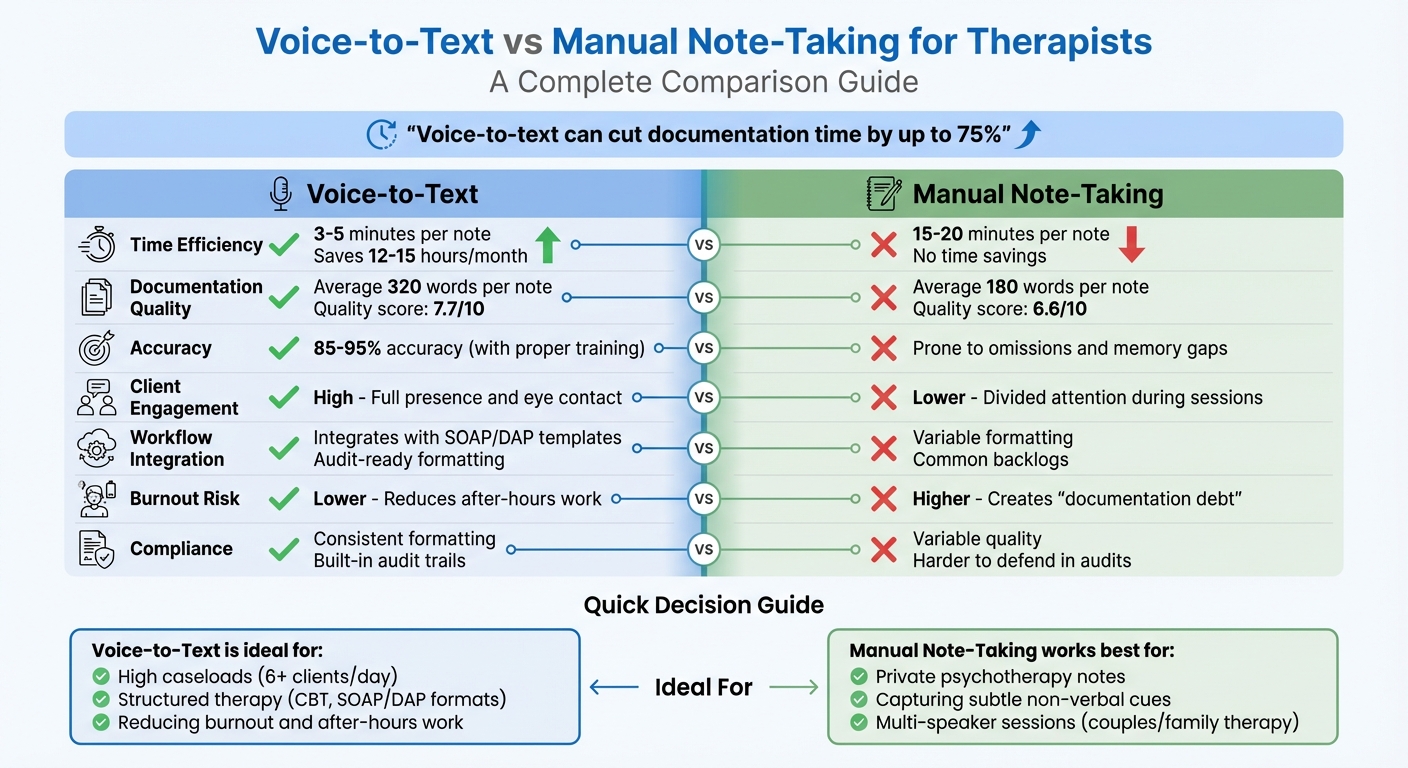
Voice-to-Text vs Manual Note-Taking for Therapists: Complete Comparison
How Voice-to-Text Technology Works
What is Voice-to-Text?
Voice-to-text technology uses AI-driven speech recognition to turn spoken words into written text. In the clinical world, specialized tools are trained on de-identified therapy data, enabling them to pick up on specific terminology and nuances that general dictation apps often miss. This allows for instant transcription into text fields.
Modern clinical tools typically follow a three-step process. First, they convert spoken words into a clear transcript. Next, advanced language models analyze the text to identify key clinical elements like symptoms and interventions. Finally, they organize the information into structured formats, such as SOAP or DAP notes, ensuring compliance with clinical documentation standards. Considering that people speak at speeds of 100 to 130 words per minute compared to typing at 35 to 40 words per minute, voice-to-text can be up to three times faster.
This speed and accuracy make voice-to-text a game-changer for efficient clinical documentation.
Benefits for Therapists
The time saved with voice-to-text tools is substantial. AI-powered note-taking can cut documentation time by as much as 75%, freeing up 12 to 15 hours per month for many clinicians. Given that 22% of clinicians spend over 10 minutes per note – and some even take up to an hour – voice-to-text can significantly reduce this burden.
These tools also come with features tailored to therapy workflows. For example, Voice CRM offers custom tags for tracking recurring themes and mood tracking to help visualize emotional trends, making the therapeutic process smoother while maintaining high-quality documentation. Advanced platforms further simplify the process by automatically formatting dictated notes into professional standards like SOAP, DAP, BIRP, or GIRP, ensuring consistency and audit readiness. Additionally, professional-grade software like Dragon Professional boasts over 95% accuracy when properly configured. Some medical-specific engines even recognize a vast array of over 50,000 medical terms, ICD-10 codes, and abbreviations right out of the box.
Security and Compliance
While voice-to-text tools boost efficiency, protecting client data remains essential. HIPAA compliance is a non-negotiable requirement for any therapy documentation tool. To safeguard client confidentiality, these platforms must use end-to-end encryption for data both in transit and at rest. Before entering client information, ensure the vendor provides a signed Business Associate Agreement (BAA), which legally binds them to protect Protected Health Information (PHI) under HIPAA guidelines.
Some advanced tools take security a step further. For instance, certain platforms employ "zero recording storage", meaning session audio is deleted immediately after transcription, minimizing risks from data breaches or subpoenas. Others include PII scrubbing capabilities to automatically redact personally identifiable information from transcripts. It’s also critical to verify that the provider doesn’t use your PHI to train their AI models unless you’ve explicitly opted in. Voice CRM, tailored specifically for psychologists, ensures data security with end-to-end encryption within a HIPAA-compliant iOS environment.
sbb-itb-ce1c1e8
Manual Note-Taking Methods
How Manual Note-Taking Works
Manual note-taking gives therapists complete control over how they document each session. Whether it’s jotting down notes with pen and paper, typing on a laptop, or using a stylus on a tablet, the therapist decides how to record their clinical impressions. This hands-on approach ensures the documentation reflects their personal clinical judgment rather than relying on automated systems for interpretation.
Common methods include traditional pen-and-paper notes, digital typing, and stylus-based input – each offering its own mix of simplicity and practical considerations. Some therapists also prefer to create typed summaries after sessions, drafting de-identified bullet points or full notes once the client has left.
"I take what are called ‘psychotherapy notes’ (bulleted points during sessions) and then create the formal session notes (also referred to as ‘progress notes’) after the client has left the session."
– Jordan Nodelman, MSW, LICSW, LCSW
This process of writing or typing encourages therapists to slow down and carefully reflect on each case, allowing them to organize their thoughts in real time. This deliberate approach helps produce objective, well-thought-out documentation.
While manual note-taking methods provide flexibility, they also come with challenges, which are explored below.
Pros and Cons
Manual note-taking stands out for its adaptability and independence. Therapists can fully control how they phrase their notes, the tone they use, and the clinical reasoning they document. This level of customization is especially valuable for expressing nuanced assessments and adapting to various clinical scenarios. Plus, because it doesn’t depend on technology, manual note-taking can be a lifesaver during home visits, emergencies, or technical failures.
Interestingly, over 80% of patients say they’re fine with their therapist taking notes on a computer or tablet during a session, with only 5% expressing dissatisfaction. However, the time investment is a major drawback. Manual note-taking can take up to 480 hours annually, which translates to a potential cost of $72,000 at an hourly rate of $150.
Security is another concern. Handwritten notes are more vulnerable to risks like theft, fire, or being misplaced. In contrast, digital notes often benefit from encryption and access logs for added protection. Additionally, the time-consuming nature of manual entry can result in documentation backlogs, forcing therapists to spend hours catching up. This situation, often referred to as "documentation debt", is a significant contributor to professional burnout.
Review of Clinical Notes AI: Mental health progress note generator
Voice-to-Text vs Manual Note-Taking: Direct Comparison
Therapists weighing their documentation options can now see a side-by-side comparison of voice-to-text tools and manual note-taking. The differences are striking, especially when you consider factors like time, quality, and workflow impact.
Voice-to-text allows therapists to complete notes in just 3–5 minutes, compared to the 15–20 minutes required for manual note-taking. This time-saving feature alone can dramatically change how therapists manage their schedules.
When it comes to the quality of documentation, voice-to-text tools also come out ahead. Dictated notes average 320.6 words, almost twice the 180.8 words found in typed notes, and they score higher for clarity and completeness – 7.7 out of 10 versus 6.6 out of 10. Still, these tools aren’t perfect. They typically achieve 85–95% accuracy when properly trained, but they can miss subtle emotional nuances or non-verbal cues that therapists often need to add manually.
The impact on workflow and burnout is another critical consideration. By cutting note completion time to just a few minutes, voice-to-text tools can save therapists 12–15 hours each month, reducing after-hours work and minimizing burnout. On the other hand, manual note-taking often leads to documentation backlogs and contributes to professional fatigue.
Here’s a quick breakdown of these differences:
Comparison Table
| Factor | Voice-to-Text / AI | Manual Note-Taking |
|---|---|---|
| Speed | 3–5 minutes per note | 15–20 minutes per note |
| Accuracy | 85–95% with proper training; may "hallucinate" details | Prone to omissions and typos |
| Detail Level | Longer, more complete notes (avg. 320 words) | Shorter notes (avg. 180 words) |
| Quality Score | 7.7/10 for clarity and completeness | 6.6/10 for clarity and completeness |
| Client Engagement | High; allows full presence and eye contact | Lower; focus divided between client and notes |
| Workflow Efficiency | High; integrates with templates (SOAP/DAP) and EHRs | Low; double data entry and backlogs common |
| Compliance | Built-in audit trails and consistent formatting | Variable; harder to defend in audits |
| Time Saved | Reclaims 12–15 hours monthly | None; adds 30% more work time to documentation |
| Burnout Risk | Low; reduces after-hours work | High; contributes to "documentation debt" |
This comparison underscores how voice-to-text tools can transform workflows and improve patient care, while manual methods often add stress and inefficiencies.
Effects on Therapy Workflow and Documentation
The way therapists document their sessions has a direct impact on their workflow. Manual note-taking often forces therapists into a difficult choice: stay fully engaged with their clients or prioritize timely documentation. Typing notes during or right after sessions can lead to therapists feeling chained to their desks, scrambling to finish before the next appointment. This adds extra stress to an already packed schedule.
This is where new tools can make a difference. Voice-to-text technology shifts this dynamic entirely. With this approach, therapists can dictate their notes while standing, walking, or even stretching. This not only supports physical movement but also lightens the mental load of documentation, contributing to overall well-being.
"When you don’t fear writing, you’re more present and engaged in your work." – Jake Walker, Founder & Owner, VoiceToNotes.ai
For therapists managing high client volumes – 25 to 30 sessions a week – efficiency is essential. Manual documentation methods can pile up, creating a backlog that contributes to burnout. On the other hand, voice-to-text tools save significant time each month, allowing therapists to focus more on their clients or even take time for personal recovery. To put it into perspective, a therapist seeing 20 clients weekly could lose about $72,000 annually in potential revenue due to time spent on manual documentation.
Beyond time savings, these tools also improve the quality and consistency of records. Systems with built-in templates like SOAP, DAP, or BIRP ensure uniform, audit-ready documentation even for therapists with heavy caseloads. In contrast, manual notes often vary in format and completeness, which can become a risk during insurance reviews or compliance audits.
Another important factor is client engagement. Using voice dictation after sessions allows therapists to remain fully present with their clients during appointments. This uninterrupted focus not only strengthens the therapeutic relationship but also leads to richer, more detailed records. These improvements in documentation quality and workflow ultimately support a more seamless and client-centered approach to therapy.
Voice-to-Text: Pros and Cons
To wrap up the comparison, let’s dive into the specific upsides and challenges of using voice-to-text technology for therapy documentation.
Advantages
Voice-to-text technology brings a level of speed that’s hard to match. While most people type around 35 to 40 words per minute, speaking naturally can generate 100 to 130 words per minute. This efficiency can save therapists a lot of time – some report gaining back over 10 hours per week on documentation tasks.
Another perk is the hands-free functionality. Therapists can dictate notes while moving around, which reduces the strain of sitting for long periods. This mobility can improve overall comfort and well-being. Tools like Voice CRM take it a step further by offering instant transcription, allowing clinicians to capture their thoughts right after a session. This ensures that key insights aren’t lost due to delayed note-taking.
Voice CRM also enhances documentation with thematic tagging, which tracks recurring topics across sessions. It integrates features like payment tracking, mood visualization, and supervision management, all within a secure, HIPAA-compliant platform. These tools make managing a practice more efficient while maintaining professional standards. However, these benefits don’t come without challenges.
Disadvantages
Despite its advantages, voice-to-text has some notable drawbacks. While AI can efficiently document session flow, structure, and interventions, it struggles to pick up on non-verbal cues like changes in tone, shallow breathing, or trembling hands. These subtle but important markers require a therapist’s direct observation and can’t be captured through dictation alone.
Audio quality plays a major role in accuracy. Background noise or a poor microphone can lead to transcription errors. Using a quiet space and a professional USB condenser microphone can help improve results. Even so, AI isn’t perfect – it can sometimes "hallucinate" or fabricate details. Early clinical AI tools showed a false narrative rate of about 1%, which means therapists must review and edit every draft to ensure it’s both legally and ethically sound.
Client consent is another important factor. Therapists need to update intake forms to inform clients about the use of AI for note-taking and offer an opt-out option. While Voice CRM addresses security concerns with end-to-end encryption and HIPAA compliance, discussing consent remains a key ethical step. Multi-speaker scenarios, such as in couples or family therapy, also pose challenges. AI often mislabels speakers, requiring therapists to spend extra time reviewing and correcting these errors.
Manual Note-Taking: Pros and Cons
Manual note-taking offers therapists a unique level of control over their documentation, allowing them to maintain their personal clinical judgment and authentic voice. Unlike automated notes, which can sometimes sound impersonal, this method enables clinicians to capture subtle nonverbal cues – like trembling hands, shallow breathing, or shifts in tone – that technology might miss. Additionally, the physical act of writing can help therapists organize their thoughts effectively.
Privacy is another key advantage. Psychotherapist Jordan Nodelman emphasizes this point: "The psychotherapy notes are my private notes and cannot be (and are not) seen by anyone, ever". These handwritten notes are kept separate from formal progress records and aren’t stored in cloud systems, reducing the risk of third-party data breaches. This level of privacy also helps create a safe, judgment-free space where clients feel more comfortable sharing deeply personal information.
However, manual note-taking has its downsides, particularly in terms of time. The process is labor-intensive and often eats into therapists’ personal time, with many spending hours after their workday to complete documentation.
Another challenge lies in maintaining accuracy and consistency. Notes written after a session depend heavily on memory, which can lead to missed details like symptoms, timelines, or important client statements. Factors like fatigue, time pressures, and individual writing styles can cause significant variations in the quality of documentation. Additionally, taking notes during a session can split the therapist’s attention, disrupting eye contact and the natural flow of conversation. This can leave clients feeling less heard and may hinder the therapeutic connection.
While manual note-taking excels at capturing clinical nuances, its demands on a therapist’s time and its potential to affect the therapeutic relationship present notable challenges. These factors are crucial to consider when deciding on the most effective documentation method.
When Voice-to-Text Makes Sense
Voice-to-text technology shines in clinical settings where efficiency and accuracy are essential. It’s particularly useful for therapists who manage demanding schedules and need to maintain high-quality documentation. Knowing when to use this tool can help therapists optimize their workflow.
For those seeing six or more clients a day, voice-to-text can make a big difference. It allows therapists to complete notes during short breaks, preventing the dreaded pile-up of documentation at the end of the day – a common contributor to burnout. This approach fits naturally with structured documentation methods, making it easier to stay on top of records.
Complex narrative documentation is another area where voice-to-text proves invaluable. For instance, when detailed progress notes are required – complete with nuanced observations and a broader vocabulary – dictation allows therapists to produce richer, more comprehensive documentation. Studies show that dictated notes average 320.6 words compared to 180.8 words for typed notes and score higher in quality (7.7 versus 6.6).
This method also supports standardized documentation protocols. Therapies like Cognitive Behavioral Therapy (CBT), which often rely on structured formats like SOAP, DAP, or BIRP, benefit from voice-to-text’s ability to capture session details reliably. This ensures therapists are prepared for legal reviews or audits while maintaining thorough and organized records.
Finally, voice-to-text can help combat cognitive fatigue. After multiple back-to-back sessions, typing or writing can feel mentally draining. Dictation offers a less taxing alternative, reducing the effort required to document while still ensuring accuracy and depth.
Conclusion
The choice between documentation methods ultimately depends on your practice’s specific needs. Voice-to-text technology offers clear time-saving benefits, cutting documentation time down to just 2–5 minutes per note and freeing up 12–15 hours each month for therapists. With over 97% word-level accuracy, HIPAA-compliant encryption, and structured templates, this tool keeps records audit-ready and efficient.
For therapists managing heavy caseloads or using structured approaches like CBT, voice-to-text can streamline workflows, ensure compliance, and lighten administrative tasks.
That said, manual note-taking still has its place. It’s particularly useful for private psychotherapy notes kept outside medical records, trauma-focused sessions where subtle non-verbal cues are critical, or sessions involving multiple participants, like couples or family therapy. Some clients may also feel more at ease with a simple notepad rather than recording equipment. Balancing these factors highlights the importance of choosing a method that supports both clinical efficiency and patient-centered care.
A hybrid approach might be the sweet spot – jotting down quick, handwritten notes during sessions while relying on voice-to-text for formal documentation. This method maintains the therapist’s presence in the session while still improving overall efficiency.
No matter the method, clinician oversight remains key. As one expert wisely puts it: "AI is a tool – the therapist ensures the finished note is accurate and defensible". Your professional judgment is what ultimately guarantees reliable and thorough documentation.
FAQs
How do I get client consent for voice-to-text notes?
When planning to record and transcribe sessions using AI tools, it’s essential to communicate transparently with your clients. Start by explaining why the sessions will be recorded and how the recordings will be handled. Be clear about:
- Usage: Describe how the recordings and transcripts will be used (e.g., for documentation, analysis, or improving services).
- Storage: Outline where and how the data will be stored, emphasizing security measures.
- Protection: Reassure clients about privacy by detailing how their information will remain confidential.
Always request explicit permission before proceeding. Ensure clients fully understand the process and feel comfortable asking questions. Once consent is given, document it thoroughly in your session notes. This step is crucial for maintaining confidentiality and adhering to legal standards, especially when working with secure, HIPAA-compliant platforms.
What should I check to ensure a voice-to-text tool is HIPAA compliant?
To confirm a voice-to-text tool aligns with HIPAA requirements, check for these key features: data encryption, availability of Business Associate Agreements (BAAs), secure data processing (either on-device or through secure cloud protocols), and removal of identifying details from transcripts. These measures are crucial for maintaining client confidentiality and adhering to HIPAA guidelines.
When should I use a hybrid note-taking approach?
A hybrid note-taking method works well for therapists who want to enjoy the hands-on feel of writing notes manually while leveraging the convenience and security of digital tools. This approach is particularly handy for quickly jotting down thoughts during a session and later organizing them in a digital format. It strikes a balance between adaptability, compliance with regulations like HIPAA, and maintaining strong client interaction, making it a smart option for therapists managing busy or multifaceted practices.



